Your doctor in 2050 isn’t working alone—and hasn’t been for decades. Beside her stands an AI that has analyzed 500 million patient cases, read every medical journal ever published, and can predict diseases years before symptoms appear.
But here’s what surprises most people: the doctor is still essential. Medicine hasn’t been taken over by machines—it’s been transformed by partnership between human wisdom and computational power that would seem magical to us today.
Welcome to healthcare where machine learning doesn’t replace the human touch—it amplifies it beyond anything we thought possible.
The Diagnostic Revolution: From Symptoms to Certainty
Remember when diagnosis meant describing symptoms, getting tests, waiting days for results, then hoping the doctor connected the dots correctly? In 2050, that’s ancient history.
The new diagnostic process:
You wake feeling slightly off—nothing specific, just not quite right. Your smartwatch has already noticed subtle changes: heart rate variability shifted 3%, sleep pattern disrupted, body temperature elevated by 0.3 degrees.
The AI monitoring your biometrics cross-references these changes against your genetic profile, family history, recent activities, environmental exposures, and 50 billion similar data patterns from other patients.
Diagnosis arrives before you finish breakfast: Early-stage viral infection, 94% probability. Immune system beginning response. Three-day progression predicted. Complications unlikely given your profile.

Treatment recommendations appear: rest protocols, nutrition adjustments, and a prescription already sent to your home medical printer. Total time from first symptom to diagnosis and treatment plan: 12 minutes.
What used to take days and multiple doctor visits now happens automatically, accurately, and early enough to prevent most complications.
Personalized Medicine: Your Unique Treatment
The era of “standard treatment” ended decades ago. In 2050, every patient gets therapy designed specifically for their genetic makeup, lifestyle, environment, and even their gut microbiome composition.
Cancer treatment exemplifies the transformation:
A patient receives a cancer diagnosis in 2050. Within hours, AI systems have:
- Sequenced the tumor’s complete genome
- Analyzed 50,000 genetic mutations
- Compared against 100 million previous cancer cases
- Predicted which treatments will work for THIS specific cancer in THIS specific patient
- Designed a personalized drug cocktail optimized for maximum efficacy and minimum side effects
- Forecasted treatment outcomes with 89% accuracy
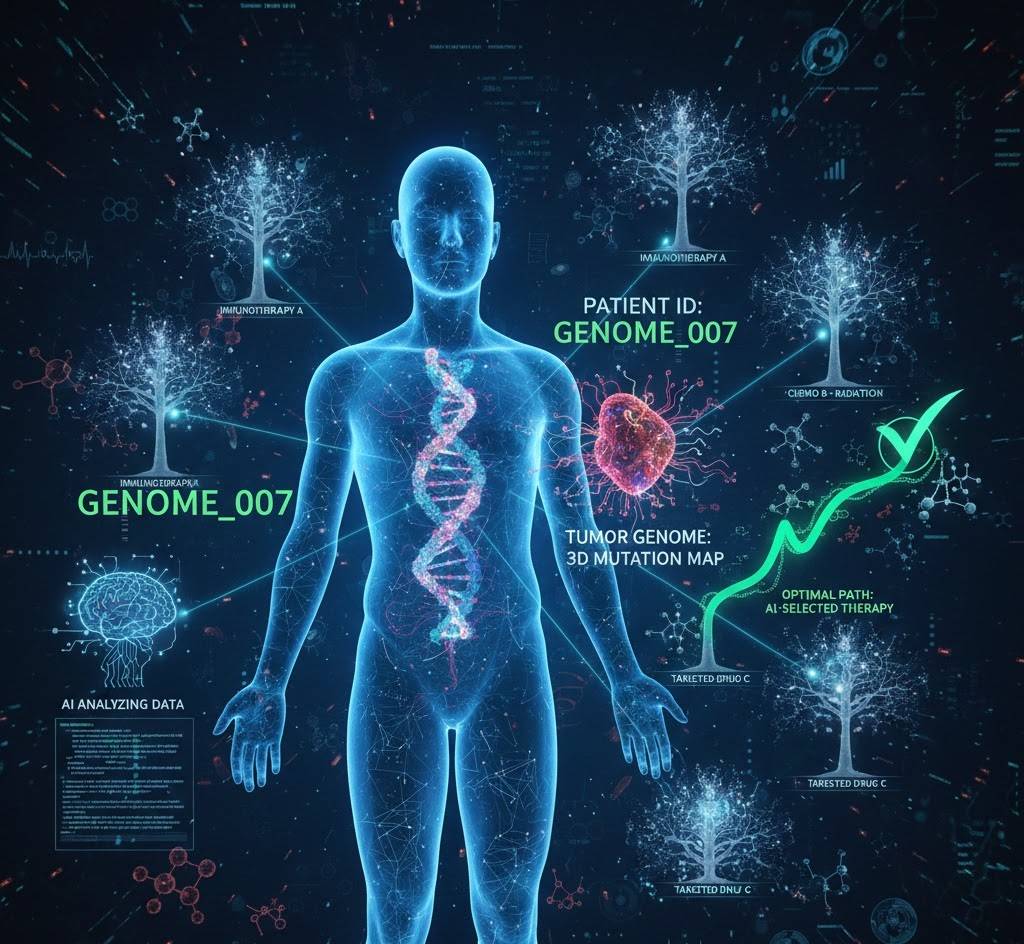
The treatment that arrives isn’t chosen from standard options—it’s created for this individual. The drug combination has never been used exactly this way before, but the AI knows it will work because it understands the molecular mechanisms with superhuman precision.
Five years earlier, this same cancer would have been terminal. In 2050, it’s a manageable chronic condition, possibly even curable.
Drug Discovery: From Decades to Days
Creating new medications used to take 10-15 years and cost billions. By 2050, AI has compressed that timeline dramatically.
The traditional process: Screen millions of molecules, test promising candidates, conduct animal trials, run human trials through multiple phases. Success rate: about 10%. Time: a decade minimum.
The 2050 process:
AI systems design molecules atom-by-atom for specific therapeutic targets. They simulate how each candidate will interact with every protein in the human body, predict side effects before synthesis, and optimize for effectiveness, safety, and manufacturability simultaneously.
Real example from 2048: An antibiotic-resistant bacterial strain emerged. Traditionally, developing a new antibiotic would take 10+ years—too late to save thousands of lives.
AI designed, tested (virtually), and optimized a novel antibiotic in 72 hours. Physical synthesis and safety confirmation took another 6 months. Total time: under a year. Lives saved: millions.
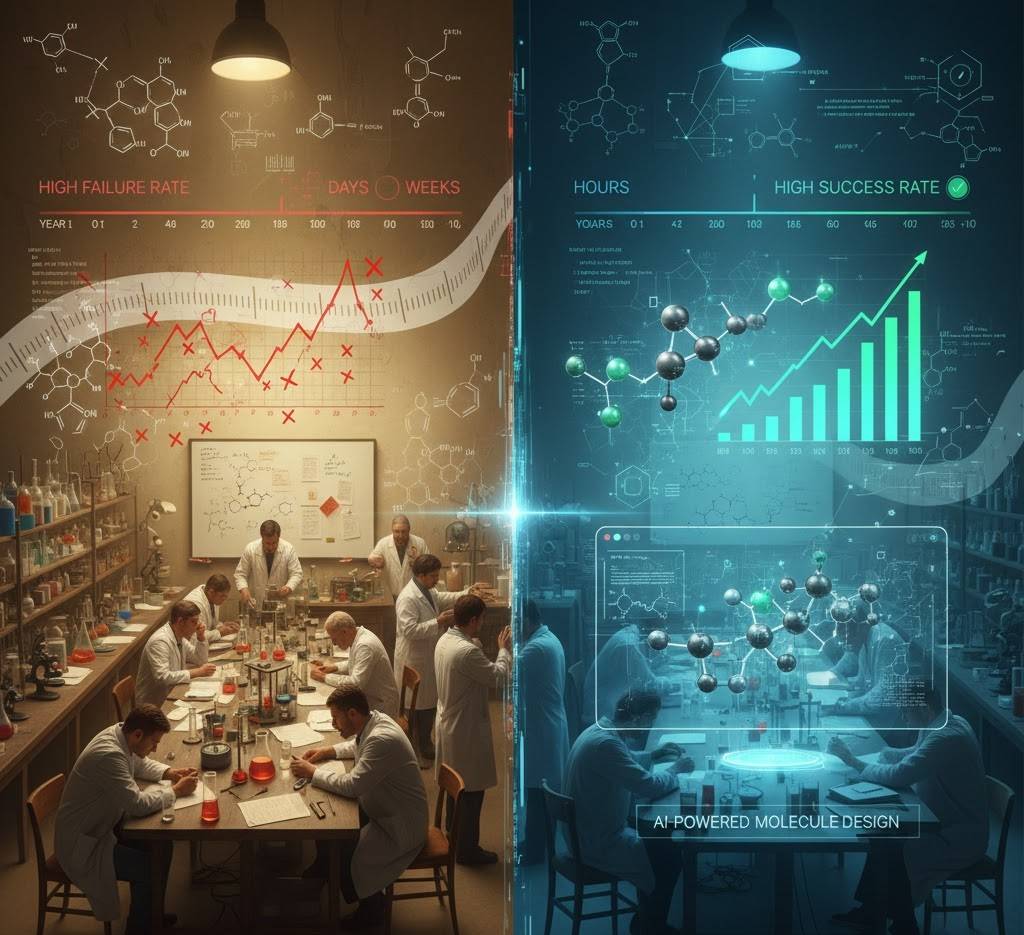
The AI didn’t just find an existing molecule—it invented one that had never existed in nature or human chemistry, optimized perfectly for the target.
Predictive Healthcare: Catching Disease Before It Starts
Perhaps most revolutionary: by 2050, we’ve shifted from reactive medicine to predictive healthcare.
Continuous monitoring systems track:
- 50+ biomarkers in real-time
- Genetic expression changes
- Microbiome composition shifts
- Environmental exposure patterns
- Behavioral health indicators
- Social determinant factors
Machine learning algorithms detect patterns invisible to humans, identifying disease risk years before conventional diagnosis would be possible.
Heart disease example:
Traditional medicine: Patient has heart attack at 55. Survives. Now on lifelong medication managing damaged heart.
2050 medicine: At age 43, AI notices subtle arterial inflammation markers, genetic variants affecting cholesterol processing, stress patterns from work, and dietary habits. Prediction: 76% probability of significant cardiac event within 12 years without intervention.

Personalized prevention program begins: specific diet adjustments, stress management protocols, targeted supplements, monitoring schedule. Result: cardiac event probability drops to 8%. Heart attack prevented.
The patient never knows they were in danger—because the danger was eliminated before it materialized.
The AI-Doctor Partnership: Better Together
Here’s what didn’t happen by 2050: doctors becoming obsolete.
What did happen: doctors becoming more effective than ever, freed from tasks machines do better while focusing on what humans do best.
AI handles:
- Pattern recognition across billions of data points
- Processing medical literature (5,000+ new papers daily)
- Remembering every drug interaction
- Monitoring thousands of patients simultaneously
- Running complex simulations
- Routine diagnosis and treatment planning
Human doctors provide:
- Empathy and emotional support
- Complex ethical decision-making
- Understanding patient values and preferences
- Dealing with ambiguity and uncertainty
- Building trust and therapeutic relationships
- Creative problem-solving for unprecedented cases

The best healthcare in 2050 comes from this partnership. AI provides superhuman analytical capabilities; humans provide wisdom, compassion, and judgment.
Surgery: Precision Beyond Human Capability
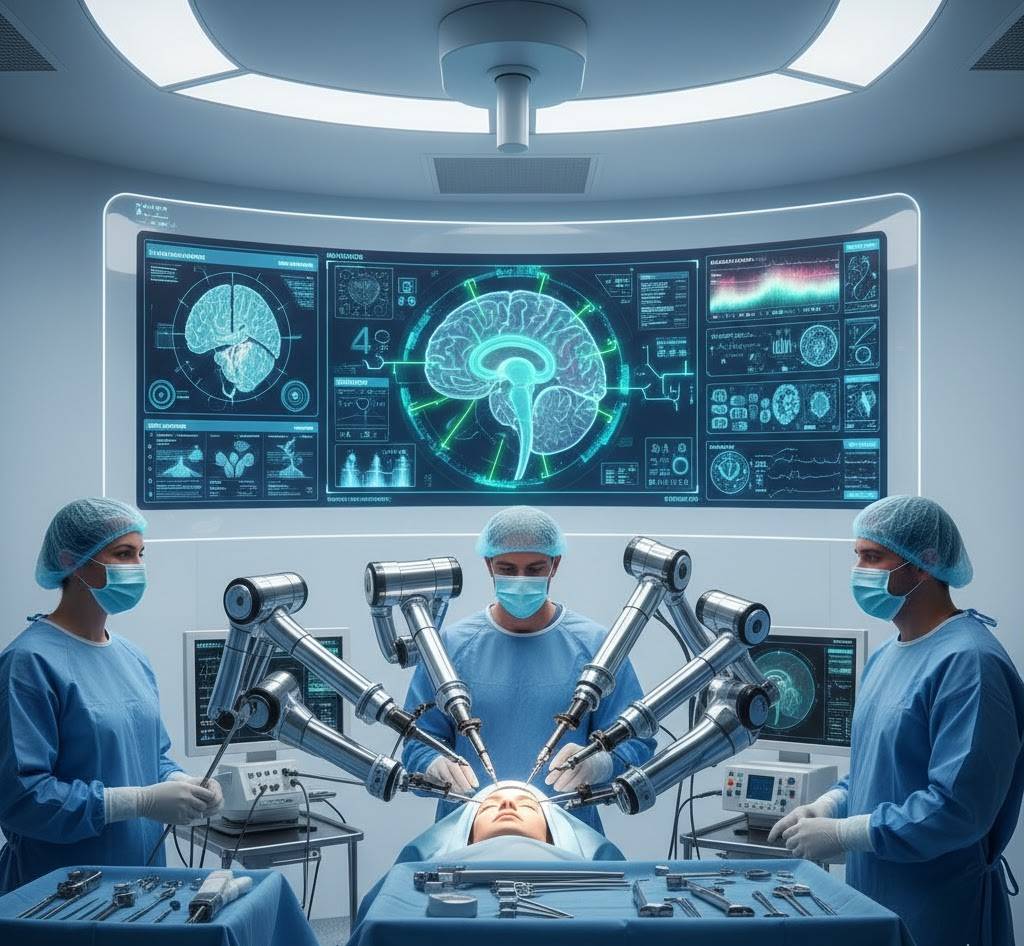
Operating rooms in 2050 look dramatically different.
Robotic surgical systems guided by AI perform procedures with precision measured in microns—far beyond human hand stability. But human surgeons remain in control, their expertise enhanced by computational assistance.
During a complex brain surgery:
The AI tracks 1,000+ variables simultaneously: blood pressure, brain activity, tissue response, instrument position, patient vitals. It predicts complications before they occur, suggests optimal approaches, and provides real-time guidance.
The human surgeon makes decisions, provides judgment for unexpected situations, and maintains ultimate responsibility. The AI makes the surgeon 10 times more effective.
Recovery optimization: Post-surgery, AI monitors healing, adjusts pain medication in real-time, predicts complications, and personalizes rehabilitation protocols. Recovery times have dropped 40% compared to 2025.
Mental Health: Understanding the Mind
Perhaps AI’s most unexpected impact is in mental healthcare—traditionally the most human-centered medical field.
Depression and anxiety treatment in 2050:
AI analyzes speech patterns, facial micro-expressions, social media activity, sleep quality, and 30+ other behavioral markers. It detects depression onset weeks before the patient consciously recognizes symptoms.
Treatment combines AI-guided therapy (available 24/7, infinitely patient, personalized to communication style) with human therapist sessions providing depth, connection, and wisdom AI cannot replicate.
Brain-computer interfaces (by late 2040s) allow direct monitoring of neural activity, enabling unprecedented understanding of mental states and precisely targeted interventions.

Suicide rates have dropped 60% since 2025—not because human connection decreased, but because early detection and intervention became possible.
Medical Education: Learning Continuously
Doctors graduating in 2050 learned differently than any previous generation.
Medical training includes:
- AI collaboration skills (as important as anatomy)
- Interpreting machine learning predictions
- Maintaining human judgment when AI suggests answers
- Ethical frameworks for human-AI decision-making
- Continuous learning (medical knowledge doubles every 73 days)
But here’s the crucial part: AI enables continuous education. Doctors don’t rely on what they learned in school—they have real-time access to latest research, global case studies, and instant expert consultation through AI systems.
The idea of a doctor being “out of date” on research becomes obsolete. Everyone has access to current knowledge immediately.

The Challenges We’re Still Solving
Despite miracles, 2050 medicine faces ongoing challenges:
Algorithmic bias: Early AI systems reflected biases in training data, providing inferior care to underrepresented populations. Constant vigilance and diverse development teams remain essential.
Privacy concerns: Continuous health monitoring generates massive personal data. Protection frameworks are robust but require eternal vigilance.
Access inequality: The digital divide could create healthcare inequality. Universal access remains a societal priority requiring active effort.
Over-reliance risk: Doctors must maintain judgment skills, not blindly trust AI recommendations.
Human connection: Ensuring technology enhances rather than replaces human interaction in healthcare remains an ongoing balance.
The Healthcare System Transformed
By 2050, these changes have restructured healthcare itself:
Hospitals handle only emergencies and complex cases. Most care happens at home with remote monitoring and AI support.
Costs have shifted—the expense of AI development and deployment is high, but dramatic efficiency gains and prevention focus have actually reduced overall healthcare spending by 30%.
Lifespan has increased to an average of 95 years in developed nations, with healthspan (years of healthy life) increasing even more dramatically.
Disease burden has shifted—infectious diseases and many cancers are now manageable or preventable. Focus has moved to aging, neurodegeneration, and rare genetic conditions.

What We Gained, What We Kept
Machine learning’s dominance in 2050 medicine doesn’t mean cold, algorithmic healthcare. Instead, it means:
Doctors spending more time with patients, not less—because AI handles routine tasks. Faster, more accurate diagnosis leading to better outcomes. Personalized treatment making every patient’s care optimal for them. Prevention replacing reaction as the primary approach.
But the heartbeat of medicine remains human: Compassion when delivering difficult news. Wisdom in complex ethical decisions. Empathy during suffering. Trust built through relationship.
AI made us better doctors. It didn’t replace the art of medicine—it freed us to practice it more fully.





